[ad_1]
When Rachel, a 35-year-old from Colorado, realized 4 years in the past that she was pregnant regardless of taking contraception drugs, she needed to verify it didn’t occur once more. The stakes have been excessive: along with not wanting children, she has a uterine deformity that makes being pregnant dangerous. She terminated the being pregnant, then started in search of long-lasting contraception.
Rachel (who requested to make use of solely her first identify to protect her privateness) lives in a rural a part of Colorado the place the one native well being system is Catholic and doesn’t supply most types of contraception beneath the Moral and Spiritual Directives for hospitals. Although Rachel had been receiving care there for years, her supplier may solely refer her to a ladies’s well being clinic an hour away when she requested about contraception strategies like diaphragms and intrauterine units (IUDs).
Although she was initially all for reversible strategies of contraception, Rachel in the end determined to have her fallopian tubes eliminated—a kind of everlasting sterilization—when she made the journey to the ladies’s well being clinic. “My first impulse when [my husband and I] obtained residence was, ‘I would like to inform each lady I do know to test your native well being system. If it’s faith-based, you could work out what meaning for you,’” Rachel says. “We came upon the arduous manner.”
Contraception is more durable to get within the U.S. than it must be. Many choices can be found—together with drugs, sterilization, and long-acting reversible contraceptives (LARCS) like IUDs—however folks incessantly wrestle to get the one they need on account of supplier refusal, insufficient insurance coverage protection, disparities in entry to care, and scientific deserts the place few reproductive well being clinicians follow.
Some well being and authorized consultants are involved that these issues might worsen sooner or later. The Supreme Courtroom’s leaked draft determination to overturn the landmark abortion entry case Roe v. Wade, which may change earlier than the Courtroom makes its remaining ruling, argues that the Structure doesn’t assure the suitable to abortion. Considered one of Roe‘s central arguments—surrounding a proper to privateness—was additionally utilized in a case that expanded entry to contraception, so some persons are involved concerning the safety of that precedent.
Within the leaked draft, Supreme Courtroom Justice Samuel Alito wrote that the choice applies solely to abortion. However after information of the draft broke, President Joe Biden stated that “each different determination regarding the notion of privateness is thrown into query.” Maryland Rep. Jamie Raskin, who can be a Constitutional scholar, raised similar fears on Twitter, writing that “if Alito’s majority destroys the suitable to privateness, states may jail ladies and medical doctors for abortion and contraception offenses.”
Lawmakers in states together with Louisiana, Idaho, and Tennessee have lately both voiced help for insurance policies that might restrict entry to some types of contraception (specifically emergency contraceptives) or denounced authorized precedent round contraceptive entry. Mississippi’s governor additionally refused to rule out the potential of future limitations on contraception entry in an interview with CNN. Latest feedback like these have raised the stakes on the subject of preserving entry to contraception.
Contraception isn’t a substitute for abortion care, says Dr. Aishat Olatunde, a Pennsylvania ob-gyn and member of the nonprofit advocacy group Physicians for Reproductive Well being. However, she says, “We wish to have the ability to make it possible for [people] have entry to all of our choices, whether or not that’s contraception, everlasting contraception, or abortion.”
The demand for long-lasting contraception
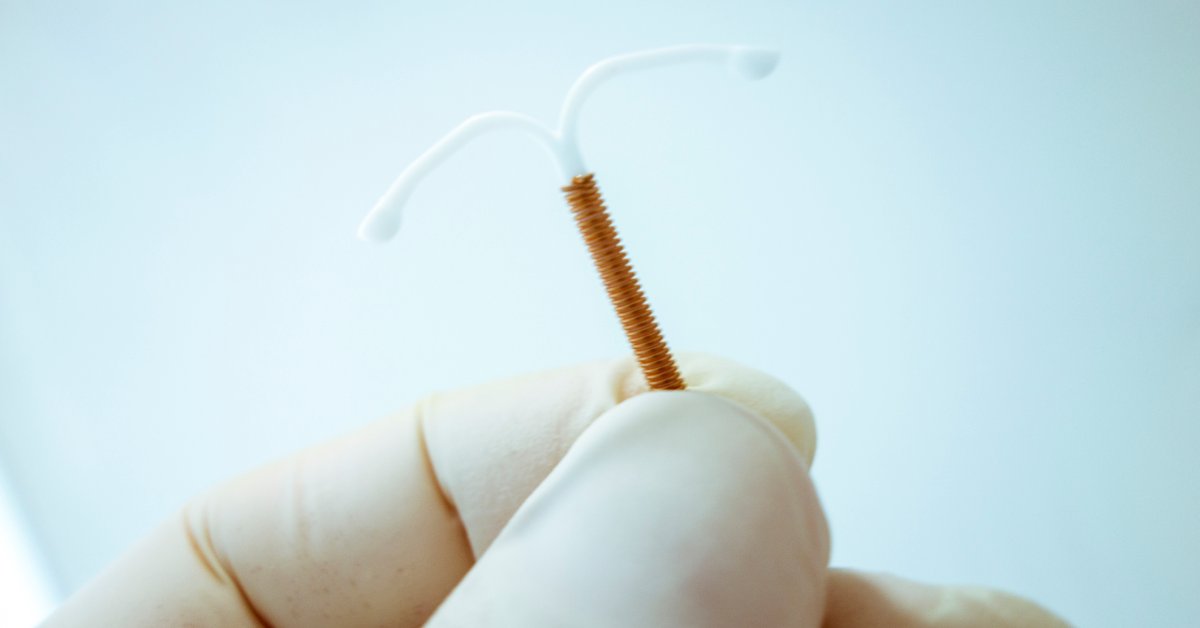
LARCs are greater than 99% efficient at stopping being pregnant, making them probably the most efficacious type of reversible contraception. This class contains IUDs: small, T-shaped units inserted into the uterus that may stop being pregnant for as much as 12 years, both by releasing low ranges of hormones or by utilizing copper to stop sperm from reaching and fertilizing eggs. One other LARC, the contraception implant, is a rodlike gadget positioned beneath the pores and skin of the higher arm that dispenses pregnancy-preventing hormones for 3 to 5 years.
LARCs have turn into much more well-liked in recent times than they was. In 2002, solely about 1.5% of U.S. ladies used them. That quantity had risen above 10% by 2017-2019, in keeping with federal knowledge —solely barely behind the 14% who used contraception drugs.
That’s largely as a result of the contraceptives have gotten safer to make use of. An IUD referred to as the Dalkon Protect grew to become well-liked within the Nineteen Seventies, nevertheless it was later linked to critical well being issues together with pelvic inflammatory illness, main physicians to cease recommending it. That left many medical doctors uneasy about recommending LARCs for years to observe. However, over time, higher merchandise have been accredited and proven to be protected.
IUDs have additionally turn into extra extensively advisable. Till 2005, the ParaGard copper IUD was solely approved for individuals who’d already had kids. After that, nonetheless, ParaGard and different IUDs have been accredited for and marketed on to youthful folks with out kids, increasing the affected person base.
Regardless of their rising recognition and spectacular efficacy, nonetheless, many individuals wrestle to entry these types of contraception.
Obstacles to contraception
Value is one impediment, says Mara Gandal-Powers, an lawyer and director of birth-control entry on the Nationwide Girls’s Regulation Heart (NWLC). Underneath the Reasonably priced Care Act, most insurers should absolutely cowl at the least one model of every kind of contraception out there within the U.S.—together with drugs, LARCs, patches (that are changed weekly), and rings (that are changed about as soon as a month). Somebody who needs an IUD ought to have the ability to get at the least one of many 5 manufacturers out there within the U.S. with out paying something.
However the NWLC’s shopper hotline receives sufficient calls from individuals who acquired large payments to know that the system isn’t working as supposed, Gandal-Powers says. Some insurers don’t adjust to the legislation, in some instances masking the contraception itself however refusing to pay for prices related to administering it or follow-up visits.
For the roughly 10% of individuals within the U.S. who’re uninsured, LARCs could also be even additional out of attain. The Mirena IUD, for instance, prices $1,049 with out insurance coverage.
The nationwide scarcity of well being care suppliers is one other drawback. Whereas contraception drugs may be prescribed nearly and delivered to many sufferers’ doorways, LARCs require an in-office go to for insertion, removing, and follow-up care. In components of the nation the place few medical suppliers and even fewer reproductive well being specialists follow, merely getting an appointment with a clinician who can place a LARC may be difficult. Half of U.S. counties didn’t have a single gynecologist working towards there as of 2017, in keeping with the American School of Obstetricians and Gynecologists (ACOG).
As Rachel realized, discovering the suitable supplier may be particularly tough in areas dominated by religiously affiliated well being care networks that may refuse to carry out reproductive care. As of 2016, roughly 16% of hospital beds within the U.S. have been in a Catholic medical middle, and in some states as many as 40% of beds are in religiously affiliated services.
Issues on the horizon
With the Supreme Courtroom’s remaining determination on Roe v. Wade looming and the way forward for contraception entry unsure, these issues might worsen. In Idaho, for instance, Republican state consultant Brent Crane stated he plans to carry hearings on banning emergency contraception, like Plan B. Crane initially stated he was not “sure” about the place he stood on entry to IUDs, earlier than strolling again that remark, the Idaho Statesman reviews.
Dr. Rachel Bervell, a medical resident who runs the Black ObGyn Venture, an internet initiative to convey anti-racism into reproductive care, says the potential overturning of Roe v. Wade raises bigger issues about limitations on bodily autonomy. “It looks like a slippery slope,” she says.
Dr. Amanda Bryson, a medical fellow at Boston Youngsters’s Hospital who has studied contraception entry, says these points are more likely to be particularly pronounced amongst folks from traditionally marginalized backgrounds, who already typically wrestle to entry equitable contraceptive care. That features folks of coloration, low-income people, people who find themselves not straight or cisgender, people who find themselves undocumented, and people who find themselves incarcerated, she says.
LARCs particularly can current sophisticated points for folks from these communities. On one hand, individuals who need long-lasting contraception might not have the ability to get it in the event that they face monetary limitations, reside distant from suppliers, or are unable to take a number of days away from work for medical appointments. However on the identical time, reproductive justice teams have voiced issues about medical doctors recommending them with out listening to affected person preferences. A 2016 joint assertion from SisterSong and the Nationwide Girls’s Well being Community, two reproductive justice organizations, warned that “an excessive amount of LARC zeal can simply flip into coercion, changing into simply the latest in a protracted line of inhabitants management strategies focused to ladies of coloration, low-income and uninsured ladies, indigenous ladies, immigrant ladies, ladies with disabilities, and folks whose sexual expression isn’t revered.”
“These are two sides of the identical coin,” Bryson says. “It comes right down to the power for anyone to have the ability to train the human proper to self-determine household planning.”
A patient-centered method is essential when providing contraception, Olatunde says. Physicians should hearken to what every individual truly needs—whether or not it’s an abortion, long-acting contraception, short-term contraception, or no contraception in any respect—reasonably than pushing their agenda.
“Medication traditionally has been this very patriarchal atmosphere the place the thought is that the physician is aware of greatest,” Olatunde says. “The truth is, we’re not in our sufferers’ sneakers.”
Whilst politicians across the nation place limits on reproductive well being care, extra clinicians are embracing affected person autonomy. In January, ACOG launched new steerage that directs clinicians to “solicit a person’s values, preferences, and perception into what issues most to them because it pertains to contraception,” echoing reproductive justice teams which have been pushing that message for years.
In March 2022, Congressional Democrats urged authorities businesses together with the U.S. Division of Well being and Human Providers (HHS) to streamline the insurance coverage protection course of for contraception, so that folks can get no matter type of contraception they need. HHS, for its half, stated in January that it’s “actively investigating” insurers’ compliance with the ACA’s requirements round contraception protection.
Altering medical tradition can go a good distance. However policy-level protections are additionally essential for preserving reproductive entry—because the Supreme Courtroom’s draft determination on abortion has proven.
That’s the message that Rachel carried away from her expertise in Colorado. “Nobody is as protected as they assume they’re,” she says. “Particularly now.”
Extra Should-Learn Tales From TIME
[ad_2]
Source link



:max_bytes(150000):strip_icc()/Health-GettyImages-StrongGlutes-d834d403c3824ecc947fd2e1272beedc.jpg)







:max_bytes(150000):strip_icc()/Health-GettyImages-1477523726-d9489f5e044241b097588b0636bf7561.jpg)

















